ESPE2016 Rapid Free Communications Pituitary (8 abstracts)
Prospective Dynamic Evaluation of Hypothalamo-Pituitary Function in 30 Cases of Paediatric Craniopharyngioma, by Hypothalamic Injury and Treatment; A Single Centre Series
Chiara Guzzetti a , Laura Losa a , Nicola Improda a , Gloria Pang a , Voraluck Phatarakijnirund a , Hoong-Wei Gan a , Richard Hayward b , Kristian Aquilina c , Ash Ederies a & Helen A. Spoudeas a
aDepartment of Paediatric NeuroEndocrinology - Great Ormond Street Hospital, London, UK; bNeurosurgery Department - Great Ormond Street Hospital, London, UK; cNeuroradiology Department - Great Ormond Street Hospital, London, UK
Background: Craniopharyngiomas are the commonest pituitary tumours of childhood. Though benign histologically, their localisation and invasive tendency can cause significant neuroendocrine morbidity and late mortality.
Objective and hypotheses: To prospectively determine risk factors for neuroendocrine morbidity by longitudinal survival analysis.
Method: All children with craniopharyngioma newly presenting to our quaternary centre between 1.8.08-9.5.15 underwent auxology, basal/dynamic pituitary function and hypothalamic invasion’s assessment by Paris grade (PG1) at diagnosis with subsequently 3–6 monthly review. We studied patient, tumour and treatment factors on progression free survival (PFS2), endocrine event-free survival (EEFS2), total endocrine morbidity score (EMS2) using Kaplan-Meier and Cox-regression statistics.
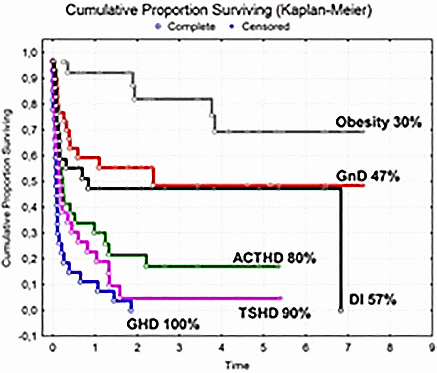
Results: In total of 30(22 M) children of median (range) age 7.6(1.1–17.2) years were followed for 4(0.3–7.4) years. Tumor volume was 16.1(1.8–193.3)cm3. 13 with presenting hydrocephalus and 11 with cysts required decompression, after which 6/22 with PG2 downgraded (n7-PG1, n3-PG0 unchanged). Surgical strategy was decompression alone (n12) or with interval resection (n7, complete(CR) n3), primary resection (n10, CRn5) or watch/wait (n1). 20 received upfront (n18) or delayed (n2) IMRT (n7) or proton (n13) radiation; just 5/30(16%) relapsed 5(1.4–5.5) years later. Outcomes: Despite 100% survival and 83.4% 5year PFS, EEFS was 0%. At diagnosis, 17/23(74%) dynamically assessed had GHD and 4/30(13%) - all intrasellar tumours - had panhypopituitarism (3 with DI). Post-treatment deficits evolved hierarchically (Figure). Presenting hydrocephalus was protective for ACTHD (P=0.04) and TSHD (P=0.006) but not for DI (P=0.04); complete resection aggravated TSHD (P=0.007) and DI (P=0.005) and transphenoidal resection aggravated GnD (P=0.0007 and ACTHD (P=0.0004). Final EMS correlated directly with total number (P=0.02), transphenoidal (P=0.02) and resection surgeries (P=0.0001), but not with PG or radiation use.
Conclusion: The evolving endocrinopathy, typical of suprasellar tumours is present from diagnosis, worse in small intrasellar tumours without mass effect and aggravated by surgical resection, but unaffected by PG or radiation. 1Puget Neurosurg 106:3–12,2007. 2Gan JCEM 100(10):3787-99,2015.
 }
}



